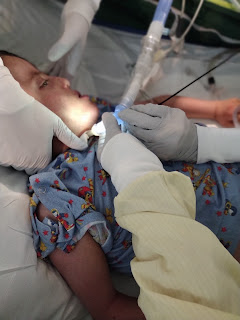
WARNING!! Do NOT read if you've experienced medical trauma, especially with your child. I'm trying to process and get things down for future reference. PTSD sucks. Just don't do that to yourself.
***************
 |
| Daddy reading stories on Tuesday |
So that last post from Monday: he DID look better in the morning, but it was early, and he was asleep, and things always look better then. Or it was the calm before the storm. Or maybe the eye of the storm. Whatever it was, it wasn't nearly as good as I hoped.
That dumpster fire? It blew up. Pretty bad.
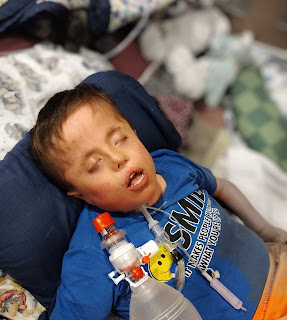
Monday he didn't want to wake up. He would respond to pain. He tried to pull away from that IV. When the RT's hands were cold, he flinched. He never opened his eyes. We did not see pupils. And he didn't shift in bed.
We took him down for CT scans, and he didn't need to be sedated. We moved him from his bed to a gurney to the machine, and then back again, and he didn't move.
While his oxygen and his temperature stayed relatively stable, that was pretty much it. That afternoon his blood pressures dropped. His skin mottled. His hematocrit, platelets, other clotting factors totally tanked. He usually has low platelets. For reference, normal platelets are 150-400 K/mcl. He usually hangs about 130-140, so just below the normal limit. Monday? 15. Yes, a 1 and a 5. With nothing else after that.
Sepsis. Flirting with DIC. Still no idea where the infection driving this is coming from.
They've done cranial, maxillofacial and thoracic CTs. Echo. Abdominal and all four limb ultrasounds. X-ray upon x-ray. Blood, sputum and other cultures both for bacteria and fungus.
When he's in the hospital, he uses a posy bed. That's the green tent-type thing you sometimes see in his hospital pictures. He uses it because he's a mover and a shaker. He'd go out through the cracks on the side rails of a normal hospital bed. It's a safety thing. Except those zippers that keep him safe also have to be undone. His team approached me about changing. We were possibly moving to where every second counted, and the posy bed became more dangerous than a regular bed. He was moved to a central location in the PICU (We'd been in the overflow area.) and they quickly and carefully moved him to a regular bed.
Fluid boluses were pushed quickly (actually before we moved) and blood was hung for rapid transfusion. They had already sent a chaplain and our ped had called me. I think they were really working to prepare me.
But here's the thing: I didn't think this was "it." I didn't like it, AT ALL!! I knew he was beyond precarious. I told our attending that if the end was coming and I didn't see it, she had to tell me. She assured me gently that she would.
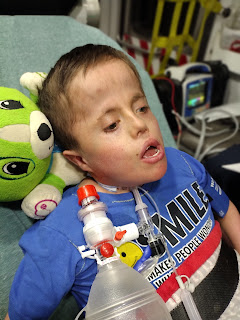
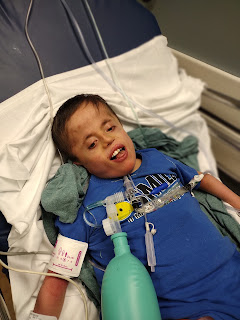
But I still felt like (and still do!) that he would pull through. I'm also very aware that this is a long, rough road back to health. He's still tenuous. It wouldn't take much to tip in the wrong direction. But today while his fever is back (again!), he's awake and interactive, and has been since last night. Yesterday, he was awake all day. He's currently on about 36 hours awake (with one 30 minute nap).
FYI: while we certainly treasures prayers, there is something else that people can do to help. That blood shortage is a very real threat. Even as bad as he was, the reason we didn't transfuse blood immediately is that it had to be processed through various channels before approval because of the extreme shortage. It took time to do that, like an hour or two. Please, please, if you can, donate blood. It WILL save lives.